As part of an overall $4.3 million grant by the Department of Defense, the Brain Electrophysiology Laboratory (BEL) Company has been awarded $1.3 million to study augmented sleep neurophysiology. The study is in partnership with colleagues at UNC School of Medicine, University of Washington, Oregon Health & Science University, University of Florida and Montana State University. If successful, this research may contribute to unique technology and intellectual property to Neurosom, Inc., the new company BEL’s founders created to commercialize advanced products for sleep assessment and therapy.

Don Tucker, PhD, CEO at BEL, and collaborators: Dr. Jeff Illif, PhD, Dr. Miranda Lim, MD, PhD, and Dr. Dawn Kernagis, PhD
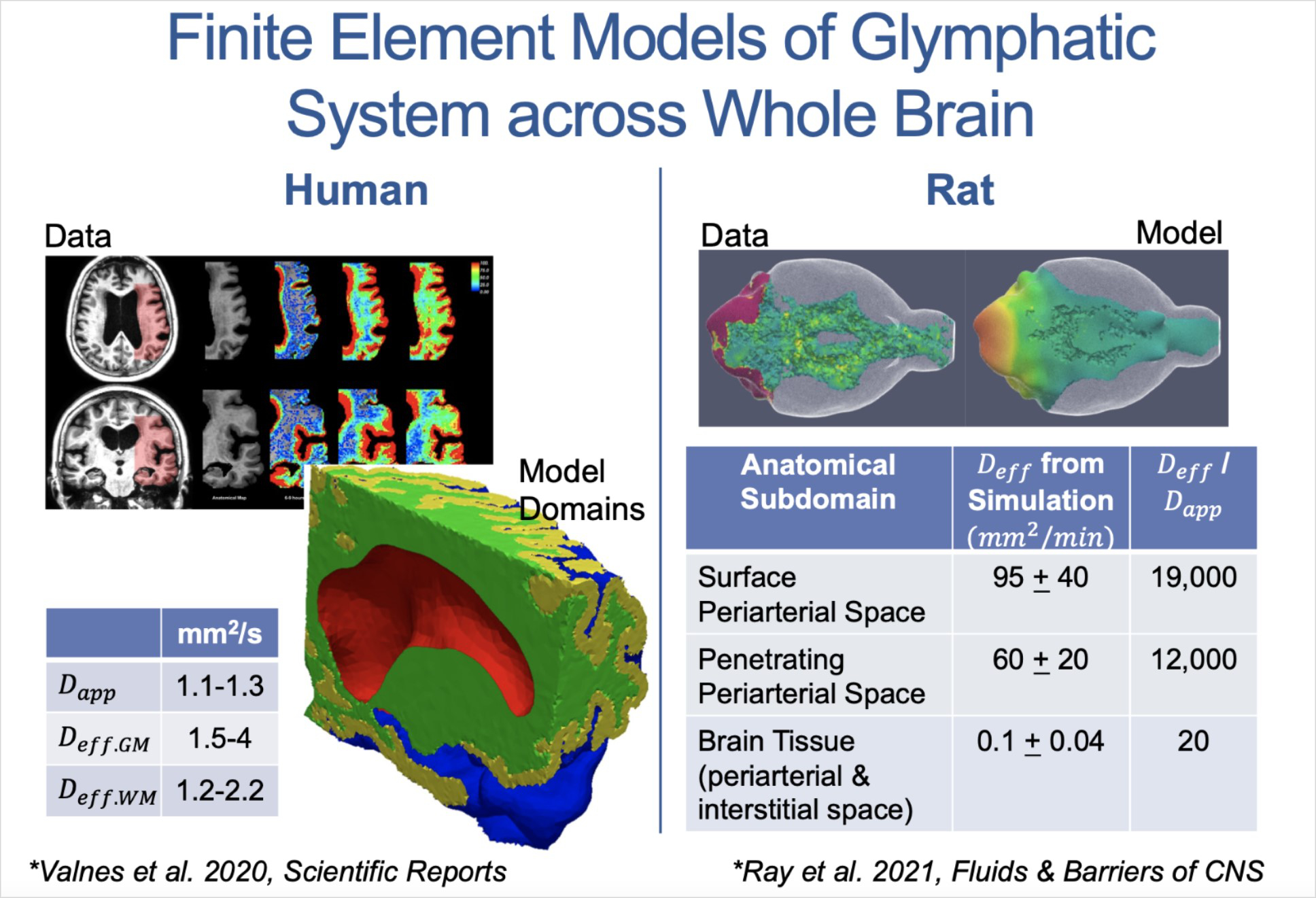
BEL collaborator Dr. Jeff Iliff and others have described the glymphatic system of the body as rapidly pushing fluids through brain tissue during sleep, facilitating the clearance of waste and plaques that accumulate during the day. (Iliff, et al, 2019) Deep sleep, or slow wave sleep (N3), is particularly important to this process, as the brain enlarges the extracellular space during deep sleep which makes the clearance more dramatic.
Glymphatic clearance is postulated to underlie the restorative effect of sleep on cognition, and the lack of it to explain the detrimental impact on cognitive power after sleep disruption. This study will use BEL technology – the Augmented Neural Oscillation Driver, or AugNOD, with TES stimulation to increase the amount of time spent in slow wave sleep for participants who are simultaneously sleep deprived. Team members will develop and test advanced MRI measurement of the glymphatic clearance of waste in the brain after sleep, with and without TES stimulation. Cognitive function will also be tested to determine if any improvement can be achieved by the additional time spent in slow wave sleep.
This landmark study could provide invaluable information on the functionality of the brain to heal itself from harmful plaques and wastes, which are linked to many neurodegenerative diseases such as Alzheimer’s. It may also provide data on improving cognitive performance of active-duty service members who are chronically sleep deprived. Additionally, the creation of non-invasive measurement using MRI of glymphatic clearance could give scientists new tools for critical neuroscience research.
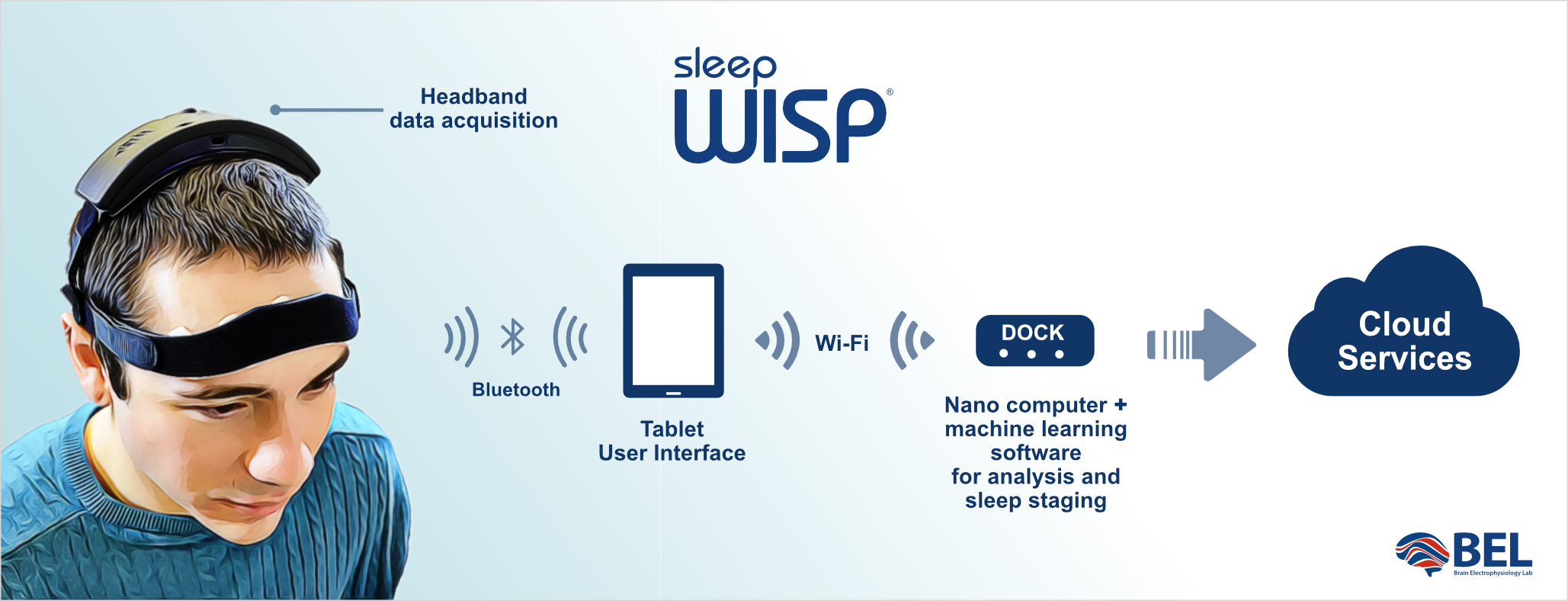
The Sleep WISP, a comfortable headband with the Home Sleep Therapy System will measure EEG activity during the night and send painless electrical currents to boost N3 sleep in the wearer. The study will test memory performance for participants before and after the sleep therapy to monitor any improvement.